Pacemaker and Defibrillator Clinic
What is a Cardiac Pacemaker?
A cardiac pacemaker is a device that is implanted under the skin which is connected to the heart by one or more pacemaker wires (“leads”) to prevent an individual from having symptoms from a heart rate that is too slow. A cardiac pacemaker maintains an adequate heart rate to ensure that adequate oxygen and nutrients flow through the body. Patients who need a pacemaker often have symptoms of lightheadedness, fatigue, fainting, and shortness of breath.
The Pacemaker Implantation Procedure
A pacemaker is implanted under local anesthesia beneath the skin on the chest usually just below the left collarbone but in some circumstances on the right side. The pacemaker leads are threaded through the subclavian vein into the heart under x-ray and tested once in position. The leads are connected to the pacemaker which is inserted under the skin through a 2-3 inch incision. Patients are often discharged home the same day. Complications are rare and include bleeding, infection or inadvertent puncture of the heart or lung (pneumothorax).
Pacemaker Follow-up
Pacemakers are followed closely in the OHVI Pacemaker Clinic. Most devices can now be monitored remotely from home using specialized equipment that comes with your pacemaker. Pacemakers last about 7-10 years and can be replaced with a minor surgical procedure when the battery becomes low, known as elective replacement indication (ERI).
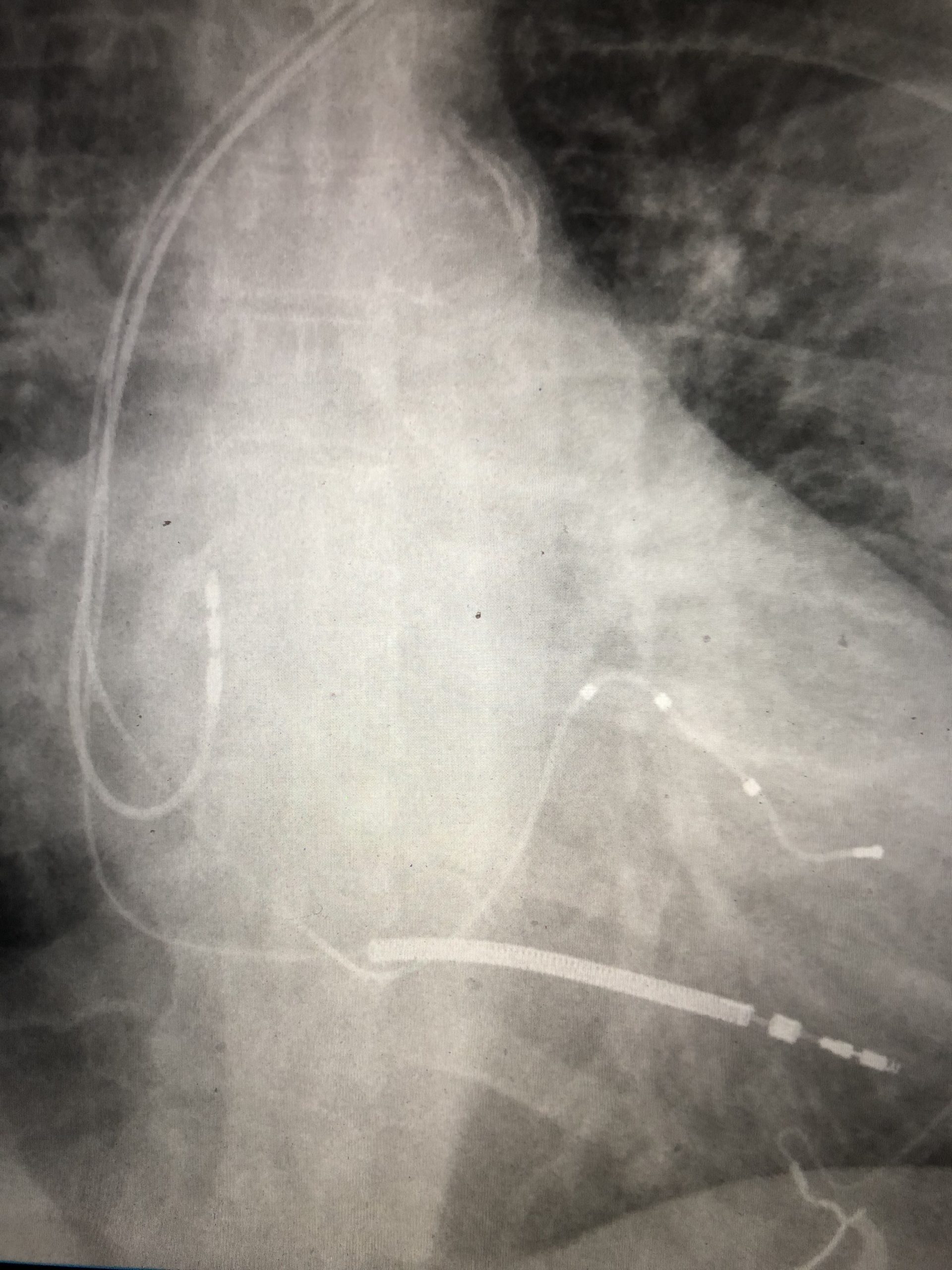
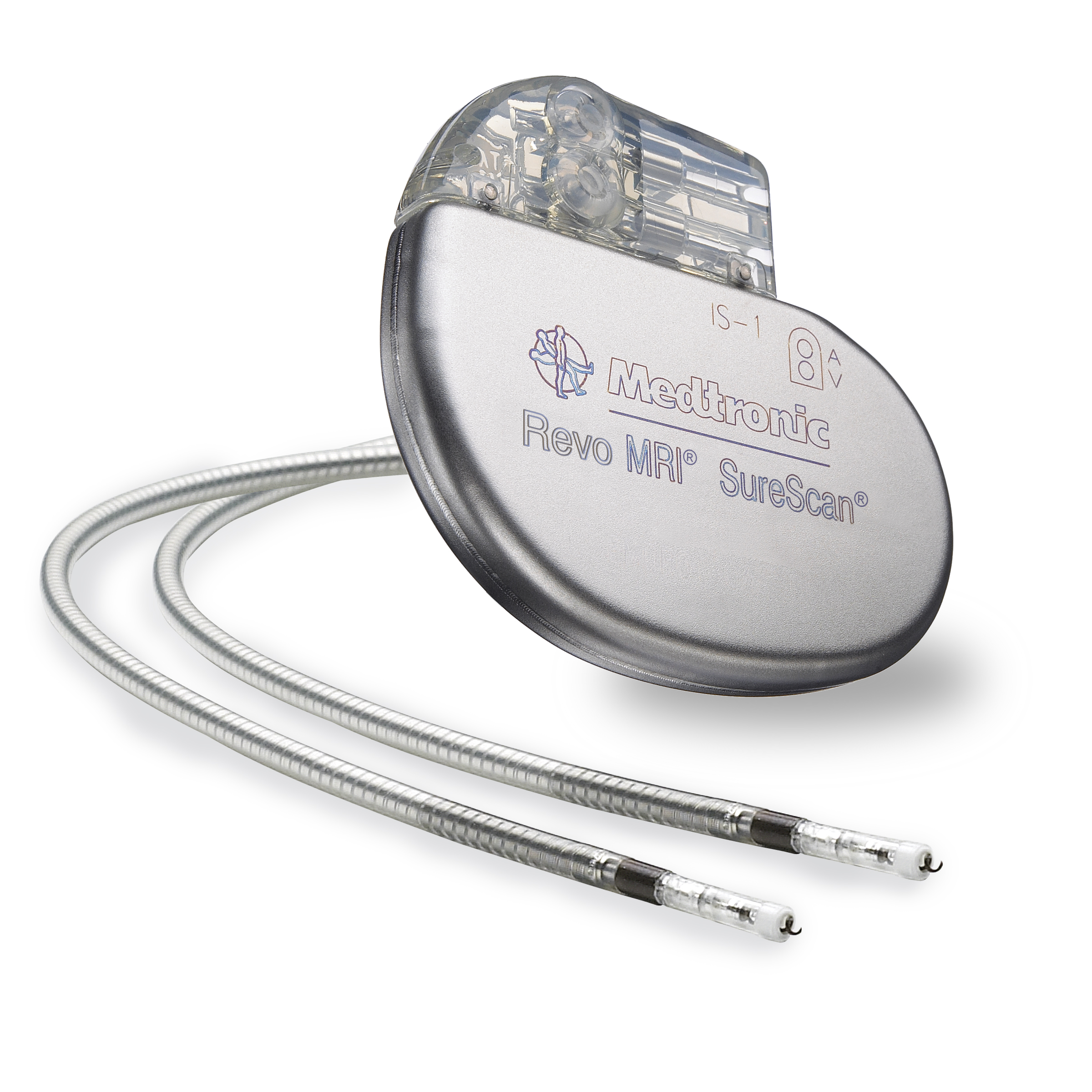
Defibrillators
An implantable cardio-defibrillator (ICD) is a pacemaker with some important added capabilities. ICD's are implanted using a surgical procedure nearly identical to pacemaker implantation. For patients who are at high risk having a fatal arrhythmia such as ventricular tachycardia or ventricular fibrillation, an ICD can detect that potentially fatal arrhythmia and automatically deliver an electric shock to the heart to restore normal rhythm thus preventing sudden cardiac death. Patients with very reduced heart pumping function or a history of ventricular arrhythmias are excellent candidates for this life-saving device.
A more advanced ICD, known as a “bi-ventricular ICD” utilizes an extra pacing lead which allows simultaneous pacing of the right and left ventricles which, in selected patients, can actually improve the cardiac pumping function and lessen symptoms of congestive heart failure. This is known as “cardiac resynchronization therapy” (CRT) and is often beneficial in patients with very advanced heart failure.
OHVI cardiologists currently implant all types of pacemakers (including new “leadless” pacemakers which are implanted directly into the heart through a catheter) and defibrillators, including bi-ventricular defibrillators. Note that many newer pacemakers and defibrillators are MRI-compatible.